Introduction:
Uterine fibroids are noncancerous growths that form in or around the uterus, affecting millions of women worldwide. These fibroids are often found in women of reproductive age, and while they are typically benign, they can cause various symptoms that affect quality of life. In this blog, we’ll explore what uterine fibroids are, how they develop, their symptoms, and available treatments.
What Are Uterine Fibroids?
Uterine fibroids, also known as leiomyomas or myomas, are benign (non-cancerous) tumors that develop in the muscle tissue of the uterus. These fibroids can range in size from tiny seedlings to large masses that can distort the shape of the uterus. They are the most common benign tumors in women of reproductive age.
While the exact cause of fibroids is not fully understood, they are believed to be influenced by a variety of factors, including genetics, hormonal imbalances, and lifestyle factors. Fibroids are typically hormone-sensitive, meaning they are often estrogen-dependent. This is why they tend to grow during the reproductive years and shrink after menopause when estrogen levels drop.
Types of Uterine Fibroids
Uterine fibroids can be classified into several types based on their location within or around the uterus:
- Intramural Fibroids: These fibroids develop within the muscular wall of the uterus. They are the most common type of fibroids and may cause heavy bleeding, pain, and pressure on the bladder or bowel.
- Submucosal Fibroids: These fibroids grow just beneath the lining of the uterus, protruding into the uterine cavity. They are less common but can lead to heavy menstrual bleeding, prolonged periods, and difficulty conceiving.
- Subserosal Fibroids: Located on the outer wall of the uterus, subserosal fibroids can grow large and press on surrounding organs, causing discomfort and pain.
- Pedunculated Fibroids: These fibroids are attached to the uterine wall by a stalk, and they can be submucosal or subserosal. Pedunculated fibroids can cause severe pain if they twist or become ischemic.
Causes of Uterine Fibroids
The exact cause of uterine fibroids remains unclear, but several factors are thought to contribute to their development:
- Hormonal Imbalances: Estrogen and progesterone, two hormones produced during the menstrual cycle, are believed to influence fibroid growth. Women with higher levels of estrogen may be more likely to develop fibroids.
- Genetics: A family history of fibroids increases the likelihood of developing them. Certain genetic mutations are thought to play a role in fibroid formation.
- Age and Reproductive Years: Uterine fibroids are most common during the reproductive years, typically affecting women between the ages of 30 and 40. The size and number of fibroids can increase during this time.
- Ethnicity: African-American women are at a higher risk of developing fibroids, and these fibroids are often larger and more symptomatic than those in other ethnic groups.
- Other Factors: Obesity, a high-fat diet, and a lack of physical activity may also contribute to the development of fibroids. Additionally, exposure to environmental toxins can play a role in fibroid growth.
Symptoms of Uterine Fibroids
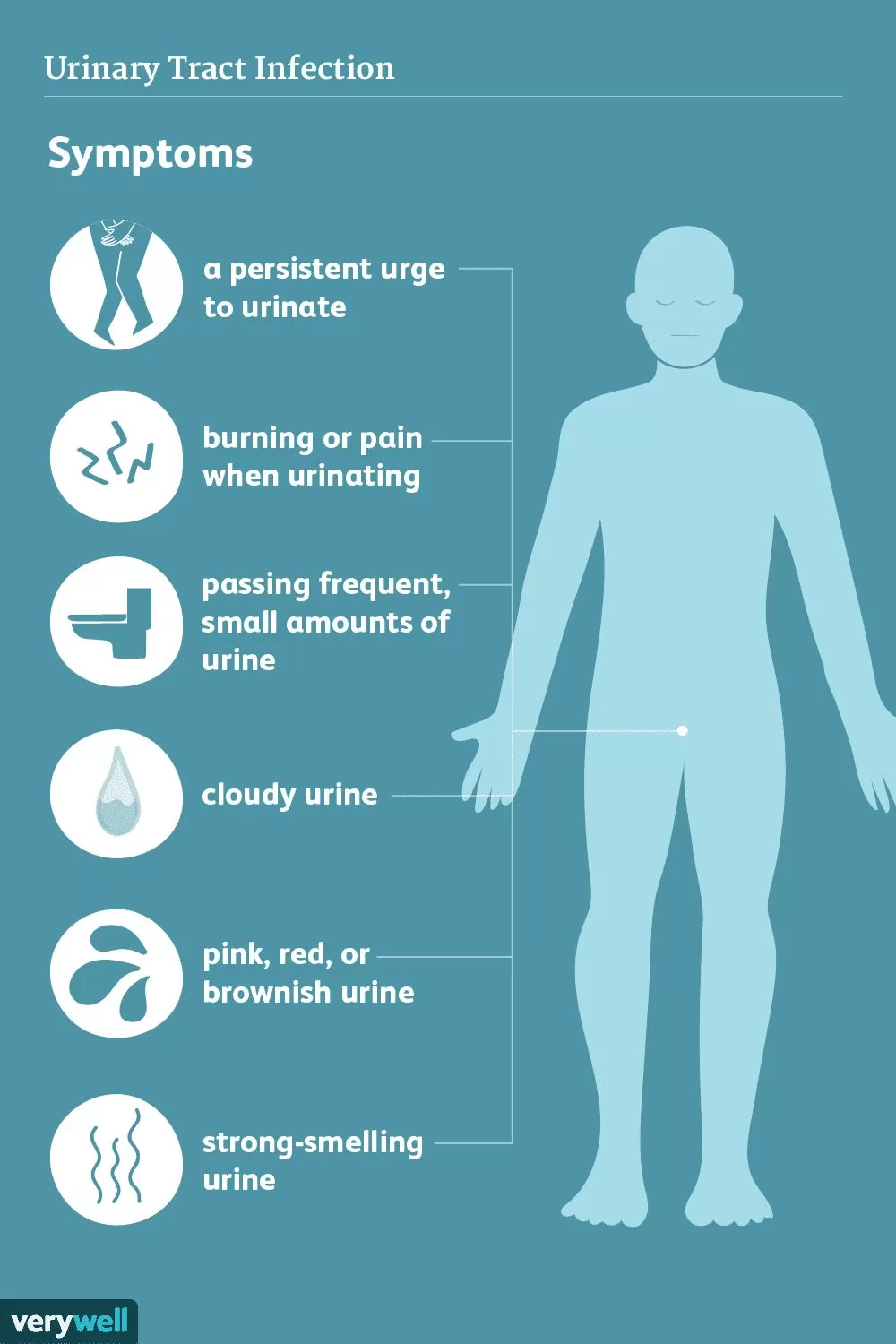
Many women with uterine fibroids may not experience any symptoms, especially if the fibroids are small. However, in some cases, fibroids can cause significant discomfort and affect a woman’s quality of life. Common symptoms of uterine fibroids include:
- Heavy Menstrual Bleeding: One of the most common symptoms of uterine fibroids is heavy or prolonged menstrual bleeding, sometimes lasting longer than a week.
- Pelvic Pain and Pressure: Large fibroids can cause a feeling of fullness or pressure in the pelvic region, leading to pain and discomfort.
- Frequent Urination: Fibroids that press on the bladder may cause increased frequency of urination or difficulty emptying the bladder completely.
- Pain During Intercourse: Fibroids located near the cervix or in the uterine cavity can cause pain during sex, especially if they are large.
- Lower Back Pain: Fibroids pressing on surrounding muscles and tissues can lead to lower back pain.
- Reproductive Issues: Fibroids can interfere with fertility by blocking the fallopian tubes or altering the shape of the uterus. They may also increase the risk of miscarriage.
- Constipation: Fibroids pressing on the rectum may cause difficulty with bowel movements and even constipation.
- Abdominal Enlargement: Large fibroids can cause noticeable abdominal swelling, which may be mistaken for pregnancy or weight gain.
Diagnosis of Uterine Fibroids
If you experience any of the symptoms of uterine fibroids, it is important to seek medical attention. A healthcare provider will perform a thorough evaluation, including:
- Medical History and Symptoms Review: The doctor will ask about your menstrual cycle, pain levels, and other symptoms related to uterine fibroids.
- Pelvic Exam: A physical exam may help identify the presence of fibroids. During this exam, the doctor may feel for any irregularities or enlarged areas in the uterus.
- Ultrasound: An ultrasound is the most common imaging technique used to diagnose uterine fibroids. It provides detailed images of the uterus and can identify the size, number, and location of fibroids.
- MRI (Magnetic Resonance Imaging): In some cases, an MRI may be used to provide more detailed images of fibroids and surrounding tissues.
- Hysteroscopy or Laparoscopy: If necessary, a hysteroscope or laparoscope may be used to examine the inside of the uterus or the pelvic cavity. These procedures are typically done under local anesthesia.
Treatment Options for Uterine Fibroids
The treatment for uterine fibroids depends on the severity of symptoms, the size and location of the fibroids, and the patient’s age and reproductive plans. Treatment options include:
- Watchful Waiting: If the fibroids are small and not causing significant symptoms, a “watchful waiting” approach may be recommended. This involves monitoring the fibroids over time without immediate intervention.
- Medications: For women who are not yet ready for surgery, medications such as hormonal therapy (birth control pills, IUDs) can help control symptoms by regulating menstrual cycles and reducing bleeding.
- Surgical Removal (Myomectomy): A myomectomy involves the surgical removal of the fibroids while preserving the uterus. This is often recommended for women who wish to retain their fertility. The type of myomectomy depends on the size and location of the fibroids.
- Hysterectomy: In more severe cases, especially for women who have completed their families and are no longer interested in preserving their uterus, a hysterectomy (removal of the uterus) may be necessary. This is the most definitive treatment for uterine fibroids.
- Minimally Invasive Procedures:
- Uterine Artery Embolization (UAE): This procedure involves blocking the blood supply to the fibroids, causing them to shrink over time.
- MRI-guided Focused Ultrasound (MRgFUS): This non-invasive treatment uses high-intensity sound waves to destroy fibroid tissue.
Managing Uterine Fibroids
In addition to medical treatments, there are lifestyle changes and alternative therapies that can help manage the symptoms of uterine fibroids:
- Diet and Exercise: Maintaining a healthy weight and exercising regularly can help manage fibroid symptoms, especially for women with larger fibroids. A diet rich in fruits, vegetables, and whole grains can support overall health.
- Stress Management: Stress can exacerbate symptoms of fibroids, so practices such as yoga, meditation, and deep breathing exercises can be beneficial for managing stress.
- Alternative Therapies: Acupuncture, herbal remedies, and other alternative therapies may help alleviate pain and reduce symptoms for some women, although it’s important to consult with a healthcare provider before trying these treatments.
Conclusion
Uterine fibroids are a common and often manageable condition that can affect a woman’s quality of life. Early diagnosis, regular monitoring, and a range of treatment options can help reduce symptoms and prevent complications. If you are experiencing symptoms of uterine fibroids, consult with your healthcare provider to determine the best course of action. With the right treatment and lifestyle adjustments, many women can successfully manage fibroids and lead healthy, fulfilling lives.
Consult us today at Oorkid Hospital and IVF Centre for expert guidance!